Sometimes it seems like there are more medicines than there are diseases, and it can be hard to keep them straight. Some can be bought over the counter at pharmacies or other stores. Others require a doctor's prescription. Some are available only in hospitals.
What Are Medicines?
Medicines are chemicals or compounds used to cure, halt, or prevent disease; ease symptoms; or help in the diagnosis of illnesses. Advances in medicines have enabled doctors to cure many diseases and save lives.
These days, medicines come from a variety of sources. Many were developed from substances found in nature, and even today many are extracted from plants.
Some medicines are made in labs by mixing together a number of chemicals. Others, like penicillin, are byproducts of organisms such as fungus. And a few are even biologically engineered by inserting genes into bacteria that make them produce the desired substance.
When we think about taking medicines, we often think of pills. But medicines can be delivered in many ways, such as:
- liquids that are swallowed
- drops that are put into ears or eyes
- creams, gels, or ointments that are rubbed onto the skin
- inhalers (like nasal sprays or asthma inhalers)
- patches that are stuck to skin (called transdermal patches)
- tablets that are placed under the tongue (called sublingual medicines; the medicine is absorbed into blood vessels and enters the bloodstream)
- injections (shots) or intravenous (inserted into a vein) medicines
No medicine can be sold unless it has first been approved by the U.S. Food and Drug Administration (FDA). The makers of the medicine do tests on all new medicines and send the results to the FDA.
The FDA allows new medicines to be used only if they work and if they are safe enough. When a medicine's benefits outweigh its known risks, the FDA usually approves the sale of the drug. The FDA can withdraw a medicine from the market at any time if it later is found to cause harmful side effects.
Different Types of Medicines
Medicines act in a variety of ways. Some can cure an illness by killing or halting the spread of invading germs, such as bacteria and viruses. Others are used to treat cancer by killing cells as they divide or preventing them from multiplying. Some drugs replace missing substances or correct low levels of natural body chemicals such as some hormones or vitamins. Medicines can even affect parts of the nervous system that control a body process.
Nearly everyone has taken an antibiotic. This type of medicine fights bacterial infections. Your doctor may prescribe an antibiotic for things like strep throat or an ear infection. Antibiotics work either by killing bacteria or halting their multiplication so that the body's immune system can fight off the infection.
Sometimes a part of the body can't make enough of a chemical. That can also make you sick. Someone with insulin-dependent diabetes, for instance, has a pancreas that can't produce enough insulin (a hormone that regulates glucose in the body). Some people have a low production of thyroid hormone, which helps control how the body uses energy. In each case, doctors can prescribe medicines to replace the missing hormone.
Some medicines treat symptoms but can't cure the illness that causes the symptoms. (A symptom is anything you feel while you're sick, such as a cough or nausea.) So taking a lozenge may soothe a sore throat, but it won't kill that nasty strep bacteria.
Some medicines relieve pain. If you pull a muscle, your doctor might tell you to take ibuprofen or acetaminophen. These pain relievers, or analgesics, don't get rid of the source of the pain — your muscle will still be pulled. What they do is block the pathways that transmit pain signals from the injured or irritated body part to the brain (in other words, they affect the way the brain reads the pain signal) so that you don't hurt as much while your body recovers.
As people get older, they sometimes develop chronic or long-term conditions. Medicines can help control things like high blood pressure (hypertension) or high cholesterol. These drugs don't cure the underlying problem, but they can help prevent some of its body-damaging effects over time.
Among the most important medicines are immunizations (or vaccines). These keep people from getting sick in the first place by immunizing, or protecting, the body against some infectious diseases. Vaccines usually contain a small amount of an agent that resembles a specific germ or germs that have been modified or killed. When someone is vaccinated, it primes the body's immune system to 'remember' the germ so it will be able to fight off infection by that germ in the future.
Most immunizations that prevent you from catching diseases like measles, whooping cough, and chickenpox are given by injection. No one thinks shots are fun. But the diseases they prevent can be very serious and cause symptoms that last much longer than the temporary discomfort of the shot. To make life easier, now you can get immunizations at many pharmacies.
Although some medicines require a prescription, some are available in stores. You can buy many medicines for pain, fever, cough, or allergies without a prescription. But just because a medicine is available over-the-counter (OTC), that doesn't mean it's free of side effects. Take OTC medicines with the same caution as those prescribed by a doctor.
Taking Medicines
No matter what type of medicine your doctor prescribes, it's always important to be safe and follow some basic rules:
- If you feel worse after taking a medicine, tell your doctor right away.
- Double-check that you have the right medicine. If you get the same prescription filled more than once, check that it's the same shape, size, and color as the last time. If not, be sure to ask the pharmacist about it.
- Read the label and follow directions. Ask if you have questions.
- Take medicines exactly as prescribed. If the instructions say take one tablet four times a day, don't take two tablets twice a day. It's not the same.
- Ask if the medicine is likely to affect everyday tasks such as driving or concentrating in school.
- Don't take more medicine than is recommended. It won't make you heal faster or feel better quicker. In fact, an overdose of medicine can make you sick.
- Always follow your doctor's or pharmacist's instructions. For instance, he or she may tell you to take a medicine with food to help lessen the stomach upset it can cause or instead to take the medicine on an empty stomach so as not to interfere with the medicine's absorption into your body.
- Never share prescription medicine with anyone else, even if that person has the same thing as you do. Today's medicines are very complex, and the dosages tend to be precisely prescribed for each person's needs. Either under-dosing or overdosing can be harmful. Additionally, someone else's body may react differently to the same medicine (for example, if the person has an allergy to one of the components of the medicine).
- If you're already taking a medicine but also want to take something you can buy over-the-counter, ask the pharmacist. There could be a bad interaction between the medicines.
- Always tell your doctor and pharmacist if you're taking any other medicines or any herbal supplements so that he or she can check for any interactions between the medicines.
- Be sure to tell your doctor if you are pregnant or might be pregnant. Some medicines can be harmful to the baby. Also, let your doctor or pharmacist know if you are breastfeeding, as some medications can cause problems with nursing.
- Remember that drinking alcohol can dramatically worsen the side effects of many medicines.
- Even if you get sick with what you think is the same old thing, don't decide on your own that you know what's wrong and take some leftover medicine. Taking that medicine for a different disease might not work — and it can even be harmful. Talk to your doctor first.
- Take antibiotics for the full length of the time prescribed, even if you start to be feel better, so that all the germs are killed and the infection doesn't bounce back.
- Keep medicines in their original labeled containers, if possible.
- Don't use medicine that has expired, especially prescription medicine.
- Medicines should not be stored in your bathroom because heat and humidity can affect the potency of the drug. Most medicines should be kept at room temperature and away from sunlight. Some must be refrigerated. Check with your pharmacist or doctor if you aren't sure.
- Make sure all medicines are stored safely and out of the reach of younger brothers or sisters and pets.
- If you have any allergies, tell your doctor and pharmacist before they start you on a new medicine.
- If you get a rash, start itching, vomiting, or have trouble breathing after starting a medicine, tell your parents immediately. Breathing difficulty, breaking out in hives, or suddenly developing swelling of the tongue, lips, face, or other body parts may be signs of a severe allergic reaction — get emergency medical care right away.
Taking medicines may feel like a hassle sometimes. But medicines are the most effective treatments available for many illnesses. If you ever have any questions about what a medicine does or how you should take it, talk with your doctor or a pharmacist.
Date reviewed: October 2018
Also found in: Dictionary, Thesaurus, Encyclopedia.
Antiviral Drugs
Definition
Antiviral drugs are medicines that cure or control virus infections.
Purpose
Antivirals are used to treat infections caused by viruses. Unlike antibacterial drugs, which may cover a wide range of pathogens, antiviral agents tend to be narrow in spectrum, and have limited efficacy.
Description
Exclusive of the antiretroviral agents used in HIV (AIDS) therapy, there are currently only 11 antiviral drugs available, covering four types of virus. Acyclovir (Zovirax), famciclovir (Famvir), and valacyclovir (Valtrex) are effective against herpesvirus, including herpes zoster and herpes genitalis. They may also be of value in either conditions caused by herpes, such as chickenpox and shingles. These drugs are not curative, but may reduce the pain of a herpes outbreak and shorten the period of viral shedding.
Amantadine (Symmetrel), oseltamivir (Tamiflu), rimantidine (Flumadine), and zanamivir (Relenza) are useful in treatment of influenza virus. Amantadine, rimantadine, and oseltamivir may be administered throughout the flu season as preventatives for patients who cannot take influenza virus vaccine.
Key terms
Cytomegalovirus (CMV) — A type of virus that attacks and enlarges certain cells in the body. The virus also causes a disease in infants.
Herpes simplex — A virus that causes sores on the lips (cold sores) or on the genitals (genital herpes).
HIV — Acronym for human immunodeficiency virus, the virus that causes AIDS.
Parkinsonism — A group of conditions that all have these typical symptoms in common: tremor, rigidity, slow movement, and poor balance and coordination.
Pregnancy category — A system of classifying drugs according to their established risks for use during pregnancy. Category A: Controlled human studies have demonstrated no fetal risk. Category B: Animal studies indicate no fetal risk, but no human studies, or adverse effects in animals, but not in well-controlled human studies. Category C: No adequate human or animal studies, or adverse fetal effects in animal studies, but no available human data. Category D: Evidence of fetal risk, but benefits outweigh risks. Category X: Evidence of fetal risk. Risks outweigh any benefits.
Prophylactic — Guarding from or preventing the spread or occurrence of disease or infection.
Retrovirus — A group of viruses that contain RNA and the enzyme reverse transcriptase. Many viruses in this family cause tumors. The virus that causes AIDS is a retrovirus.
Shingles — An disease caused by an infection with the Herpes zoster virus, the same virus that causes chickenpox. Symptoms of shingles include pain and blisters along one nerve, usually on the face, chest, stomach, or back.
Virus — A tiny, disease-causing structure that can reproduce only in living cells and causes a variety of infectious diseases.
Cidofovir (Vistide), foscarnet (Foscavir), and ganciclovir (Cytovene) have been beneficial in treatment of cytomegalovirus in immunosupressed patients, primarily HIV-positive patients and transplant recipients. Ribavirin (Virazole) is used to treat respiratory syncytial virus. In combination with interferons, ribavirin has shown some efficacy against hepatitis C, and there have been anecdotal reports of utility against other types of viral infections.
As a class, the antivirals are not curative, and must be used either prophylactically or early in the development of an infection. Their mechanism of action is typically to inactivate the enzymes needed for viral replication. This will reduce the rate of viral growth, but will not inactive the virus already present. Antiviral therapy must normally be initiated within 48 hours of the onset of an infection to provide any benefit. Drugs used for influenza may be used throughout the influenza season in high risk patients, or within 48 hours of exposure to a known carrier. Antiherpetic agents should be used at the first signs of an outbreak. Anti-cytomegaloviral drugs must routinely be used as part of a program of secondary prophylaxis (maintenance therapy following an initial response) in order to prevent reinfection in immunocompromised patients.
Recommended dosage
Dosage varies with the drug, patient age and condition, route of administration, and other factors. See specific references.
Precautions
Ganciclovir is available in intravenous injection, oral capsules, and intraoccular inserts. The capsules should be reserved for prophylactic use in organ transplant patients, or for HIV infected patients who cannot be treated with the intravenous drug. The toxicity profile of this drug when administered systemically includes granulocytopenia, anemia and thrombocytopenia. The drug is in pregnancy category C, but has caused significant fetal abnormalities in animal studies including cleft palate and organ defects. Breast feeding is not recommended.
Cidofovir causes renal toxicity in 53% of patients. Patients should be well hydrated, and renal function should be checked regularly. Other common adverse effects are nausea and vomiting in 65% or patients, asthenia in 46% and headache and diarrhea, both reported in 27% of cases. The drug is category C in pregnancy, due to fetal abnormalities in animal studies. Breast feeding is not recommended.
Foscarnet is used in treatment of immunocompromised patients with cytomegalovirus infections and in acyclovir-resistant herpes simples virus. The primary hazard is renal toxicity. Alterations in electrolyte levels may cause seizures. Foscarnet is category C during pregnancy. The drug has caused skeletal abnormailities in developing fetuses. It is not known whether foscarnet is excreted in breast milk, however the drug does appear in breast milk in animal studies.
Valaciclovir is metabolized to acyclovir, so that the hazards of the two drugs are very similar. They are generally well tolerated, but nausea and headache are common adverse effects. They are both pregnancy category B. Although there have been no reports of fetal abnormalities attributable to either drug, the small number of reported cases makes it impossible to draw conclusions regarding safety in pregnancy. Acyclovir is found in breast milk, but no adverse effects have been reported in the newborn. Famciclovir is similar in actions and adverse effects.
Ribavirin is used by aerosol for treatment of hospitalized infants and young children with severe lower respiratory tract infections due to respiratory syncytial virus (RSV). When administered orally, the drug has been used in adultys to treat other viral diseases including acute and chronic hepatitis, herpes genitalis, measles, and Lassa fever, however there is relatively little information about these uses. In rare cases, initiation of ribavirin therapy has led to deterioration of respiratory function in infants. Careful monitoring is essential for safe use.
The anti-influenza drugs are generally well tolerated. Amantadine, which is also used for treatment of Parkinsonism, may show more frequent CNS effects, including sedation and dizziness. Rapid discontinuation of amantidine may cause an increase in Parkinsonian symptoms in patients using the drug for that purpose. All are schedule C for pregnancy. In animal studies, they have caused fetal malformations in doses several times higher than the normal human dose. Use caution in breast feeding.
Interactions
Consult specific references for information on drug interactions.
Use particular caution in HIV-positive patients, since these patients are commonly on multi-drug regimens with a high frequency of interactions. Ganciclovir should not be used with other drugs which cause hematologic toxicity, and cidofovir should not be used with other drugs that may cause kidney damage.
Resources
Periodicals
Gray, Mary Ann. 'Antiviral Medications.' Orthopaedic Nursing 15 (November-December 1996): 82.
antiviral
2. an agent effective against viruses.
antiviral drugsmay be useful in early stages of some virus infections or to prevent recurrences or reactivation in chronic infections. Most drugs exert their effects only during certain stages of viral replication and many are relatively toxic for the host when used systemically. In general, chemotherapy of virus infections in animals is uncommon with limited applications, mainly in topical treatment of ophthalmic infections. Examples are idoxuridine, vidarabine, amantadine hydrochloride, acyclovir, ribavirin.
Want to thank TFD for its existence? Tell a friend about us, add a link to this page, or visit the webmaster's page for free fun content.
Link to this page:
(CBS News) Illicit drugs are bad for you. Almost every doctor will recommend avoiding recreational drug use, because it can lead to long-term health problems and drug abuse that can ruin personal relationships and even send a person to an early grave.
But while drugs can be dangerous, illicit drugs have been researched for centuries, and some have been found to have surprising therapeutic benefits.
Whether it's a psychological benefit or treating an addiction to one drug with the help of another, several studies document the potential medicinal effects of otherwise illegal drugs.
Medical Drugs And Their Uses Teluguwap
Keep clicking to see 7 drugs that researchers have found might have a medicinal uses..
Surprising medical uses for illicit drugs
LSD (Acid)
Lysergic acid diethylamide, known as LSD or acid, comes in tablets, capsules, liquid, or on absorbent paper (pictured left). The hallucinogenic drug produces 'trips' that last about 12 hours and involve unpredictable feelings of panic and fright. Although LSD raises body temperature, heart rate and blood pressure, and has even been linked to 'flashbacks' months after use, it may have a sobering effect on alcoholics, according to a recent study.
The study found people with alcohol problems who took LSD reported greater self-acceptance, awareness and motivation to address their alcohol abuse.
Surprising medical uses for illicit drugs
Marijuana
The most commonly used illegal drug in the U.S. has found many purposes - recreational, spiritual, and medicinal. Uncle Sam even doles out free joint canisters to four Americans who were grandfathered into an experimental government treatment study that looked at marijuana for medicinal reasons. Others are simply authorized to grow medical marijuana on their own. Marijuana has been found to relieve chronic pain, prevent post-traumatic stress disorder, and has even found celebrity advocates such as TV personality Montel Williams.
Currently 16 U.S. states and Washington D.C. have medical marijuana laws on the books.
But marijuana use has also been tied to long-term brain problems, risk for psychotic symptoms, and deadly car crashes.
Surprising medical uses for illicit drugs
MDMA (Ecstasy)
MDMA, known as ecstasy, XTC or X, is a synthetic drug that produces short-term feelings of emotional warmth, physical energy, and enhanced sensory perception. But it can also cause nausea, chills, muscle cramping and blurred vision. The drug, which grew in popularity as a club drug, was found to potentially hold the key to better treatments for deadly blood cancers such as leukemia, lymphoma, and myeloma.
Another study found MDMA combined with therapy could help treat post-traumatic stress disorder (PTSD).
Surprising medical uses for illicit drugs
Cocaine
Cocaine, known in its crystal form as 'crack,' is a highly addictive stimulant that is snorted, injected, or smoked. It produces feelings of euphoria while increasing body temperature, blood pressure, and heart rate - thereby also raising risk for heart attacks, respiratory failure, strokes and seizures. Sudden death can occur on the first use of cocaine.
Despite its dangers, cocaine has a history of medicinal use, once used as a stimulant for those wasting away from disease or morphine addiction - the latter was especially common following the Civil War - and thought to be a general cure-all, sold as tonics by pharmacists. Cocaine was also one of the earliest anesthetics used for surgery. Some current anesthetics, such as novocaine, use safer versions of the chemical without the psychological effects.
Surprising medical uses for illicit drugs
Psilocybin (Magic mushrooms)
Psilocybin is a hallucinogen found in certain kinds of fungus, commonly known as psychedelic or magic mushrooms. While consuming these mushrooms produces short-term drug 'trips,' research has found that magic mushrooms may lead to a long-term greater sense of well-being and help treat depression.
Another study found the drug could give people a more 'open' personality, making them more likely to quit smoking or treat anxiety and depression in cancer patients.
'We're not saying go out there and eat magic mushrooms,' Professor David Nutt, a neuropsychopharmacology researcher at Imperial College London and magic mushroom study author said. 'But..this drug has such a fundamental impact on the brain that it's got to be meaningful - it's got to be telling us something about how the brain works.'
Surprising medical uses for illicit drugs
Ibogaine
Ibogaine is a hallucinogenic drug that's found in African Iboga shrubs and is commonly taken for religious rituals. Despite it being a powerful hallucinogen that's illegal in the U.S., some addiction doctors in other countries are turning to the plant to treat heroin and opioid addiction.
One ibogaine researcher, Dr. Kenneth Alper of NYU Langone Medical Center, told HealthPop last summer that the approach is mostly used for people who fail more conventional treatments. The drug is thought to work for addicts by helping them through potentially deadly withdrawal symptoms, and reportedly changing drug-seeking behavior in some addicts.
Surprising medical uses for illicit drugs
Ketamine
Ketamine, also known as 'Special K,' is a club-drug that puts users in a trance-like state known as a 'K-hole.' The drug is commonly used as a cat tranquilizer by veterinarians, and may cause visual hallucinations, vivid dreams, confusion and disorientation, increased salivation, and problems with heart rhythm and breathing.

But a recent study of depressed patients at Ben Taub General Hospital in Houston found the drug treated people with suicidal depression during the critical stretch when depressed patients were most vulnerable.
'It was a different experience from feeling high. This was feeling that something has been removed,' said Dr. Carlos Zarate, a ketamine researcher at the National Institute of Mental Health.
These are the drugs normally classed as club drugs.
- Ecstasy
- GHB
- Ketamine
- Rohypnol
- LSD
- Methamphetamine
There are several other synthetics substances that may be fraudulently sold as Ecstasy or that may be abused in a club environment, either in the US or other countries. These drugs include:
- Piperazines like BZP and TFMPP
- PMA/PMMA
- Mephedrone (mostly outside the US)
- bk-MDMA (methylene)
- MDPV
- Ecstasy:
Ecstasy
Ecstasy is the most popular drug in this class. It is referred to as an empathogen or entactogen. These two terms are used interchangeably to describe a drug that creates artificial feelings of empathy. In other words, they make a person feel deeply close to someone else that they may have just met.
Ecstasy is usually handed out in small colored pills that are often stamped with a logo or character’s image. These may be loose or enclosed in a blister pack. Ecstasy also comes in a crystal or powdered form and occasionally a liquid.
Ecstasy effects:
- Greater enjoyment of dancing
- Distortions of perceptions, particularly light, music and touch
- Artificial feelings of empathy and emotional warmth
- Euphoria
- Increased body temperature, blood pressure and heart rate
- Threat of dehydration
- Increased energy
- Lack of appetite
- Lack of fatigue when it would be normal
- Jaw clenching and teeth grinding
- Chills
- Muscle cramping
After Ecstasy’s immediate effects have worn off, some people, especially heavy users, complain of:
- Anxiety
- Restlessness
- Irritability
- Sadness
- Lack of appetite
- Less interest in or pleasure from sex
- Problems sleeping
- Aggressive behavior
- Difficulty focusing
- Poor memory
- Drug cravings
- Paranoia
Effects of Ecstasy usually last between three and six hours although it is common for people to take more as the effects start to wear off so they can continue the experience.
Because Ecstasy is a strong stimulant, it makes a person’s body overactive. Without sufficient cooling and water, it is easy for an Ecstasy user to overheat after dancing the night away. Some nightclubs have chilling rooms that are highly air conditioned, that also sell cold water. Some Ecstasy users know that they need to stay hydrated and cooled. When Ecstasy is combined with alcohol, as it often is, the tendency for dehydration is even more pronounced.
An Ecstasy overdose can also make a person overheat. A person’s temperature can soar to 109 degrees F (42.8 degrees Celsius) or even higher if they have overdosed on Ecstasy. This high temperature causes organ failure and death. An overdose can also cause seizures and fainting.
One of the effects of Ecstasy is addiction. Some people will begin by using Ecstasy on the weekends, but after a period of use, find themselves deeply depressed in the middle of the week. They may make it to the weekend before using more but then finally start using Ecstasy daily to try to lift the depression. They are now addicted.
Ecstasy nicknames: Ecstasy, E, X, XTC, the Hug Drug, Love Drug, Disco Biscuit, Adam, Clarity, Lover’s Speed, rolldogs, E-tarts, Scooby Snacks. Crystalline or powder Ecstasy is called Molly
One of the problems with abuse of Ecstasy is that few of the pills sold as Ecstasy contain only this drug. They may be diluted or adulterated with MDA, PMA, ketamine, PCP, dextromethorphan, ephedrine, pseudoephedrine, amphetamine, methamphetamine, cocaine or caffeine. Some pills may contain no Ecstasy at all.
While it might seem harmless to include caffeine in one of these pills, if a person takes caffeine with methamphetamine, it is easier for them to become overheated to a life-threatening degree.
GHB
GHB is short for gamma-hydroxybutyric acid or gamma-hydroxybutyrate. GHB is a central nervous system (CNS) depressant that is administered as a liquid, pill, capsule or powder. Effects last up to four hours. As a CNS depressant, GHB slows the heart and breathing to potentially dangerous levels. It is a sedative and causes euphoria and anesthesia. When mixed with alcohol, its effects are even more dangerous.
Some bodybuilders have used this drug as it is thought to help them get reduce body fat. It is mainly used recreationally or as a date rape drug as it induces a feeling of relaxation. It has no odor and no taste.
GHB effects:
- Euphoria
- Sedation
- Confusion
- Dizziness
- Hallucinations
- Lowered inhibitions
- Short-term amnesia
- Combativeness
- Dilated pupils
- Involuntary eye movement
Adverse effects, including those of overdose:
- Vomiting
- Nausea
- Seizures
- Tremors
- Disorientation
- Incontinence
- Low body temperature
- Fatal respiratory problems
- Coma
- Liver failure
- Death
GHB nicknames: Liquid X, Liquid Ecstasy, scoop, soap, grievous bodily harm, Georgie home boy, G-caps, everclear, G, smart drug, vita G.
GHB has very limited medical use. Any other use is illegal.
Ketamine
Ketamine is primarily used as a veterinary anesthetic. It was developed as a human anesthetic, but its use was largely discontinued after patients had too many adverse effects, including delirium, irrational behavior, hallucinations and confusion. It is occasionally still used as an anesthetic for a person who is injured but can’t be moved, for example, when they have a bad car accident and are trapped in the damaged car. In this situation, it would be dangerous to slow down a person’s breathing or make their blood pressure drop, as could happen if they were given morphine. Emergency medical technicians may give ketamine at times like these.
Ketamine is a dissociative drug, which means that a person abusing it loses touch with his own thoughts and identity. He (or she) may feel that someone else is having his thoughts. He may feel completely separated from his own body. A state of complete dissociation is sought by some addicts. They will keep taking more of the drug until they reach this state, called the “k-hole.”
Ketamine effects:
- Distortion of sight and sound
- Feelings of detachment from the environment and oneself
- Illusions
- Hallucinations
- Nausea
- Slowed breathing
- Vomiting
- Dizziness
- Confusion
- Slurred speech
- Sedation
- Numbness
- Weakness
- Visual problems
- Muscle rigidity
- Aggressive behavior
- Loss of coordination
- Rapid heart rate
- Amnesia
- Delirium
Hallucinatory effects of ketamine last an hour or less, but a user’s judgment, coordination and perception may be affected for much longer. Some people suffer flashbacks after using this drug. It is possible to die from an overdose of ketamine. Ketamine can be injected, snorted or smoked. It is sometimes mixed with marijuana and smoked.
Ketamine may be used as a date rape drug. It is tasteless and odorless. A person raped after being given ketamine may not even remember that it happened.
Ketamine nicknames: Special K, Vitamin K, Super K, Ketaset, Jet, Super Acid, cat valium, honey oil, Kit Kat, K, Special La Coke
Use of ketamine with other drugs, including alcohol, benzodiazepines like Xanax, barbiturates or opiates is particularly dangerous and can result in death. Heavy use of ketamine can result in damage or even destruction of the bladder, resulting in severe pain during urination and need for surgical removal of the bladder.
Ketamine is frequently stolen from veterinary clinics. Its use is highly restricted and illicit use is illegal.
Rohypnol
The generic name of Rohypnol is flunitrazepam. It is a type of benzodiazepine, the same class of drug as Xanax and Valium. This drug is ten times the strength of Valium.
The drug is illegal in the US but is available over the counter in Mexico and by prescription in many other countries.
It takes effect very quickly. Rohypnol is broken down and passed from the body quickly. Many people think this means that it cannot be detected on a drug test. This feature increases its popularity. In fact, it can be detected 72 hours later but some drug tests do not include a screen for this drug.
When used for date rape, Rohypnol is usually slipped into an alcoholic drink. It has no taste or odor. It has recently been released in a new formulation intended to prevent this drug from being used for date rape. It now comes as a green pill that turns blue when it is dissolved in a drink. An older white pill is being phased out of use by its manufacturer Hoffman-La Roche.
When the drug is simply being abused, most people swallow or chew the tablets or let them dissolve under their tongues. Or they may crush the pills and snort them, mix them with marijuana and smoke them, or dissolve them and inject the solution. Strong effects may last six hours but residual effects may still be present twelve hours later. Mixing Rohypnol with alcohol is particularly dangerous.
Rohypnol nicknames: Roofies, Rophies, Rope, Roach-2, Lunch Money Drug, Mexican Valium, Forget Me Pill, Wolfies, Ruffles, Robutal, La Rocha, Circles, Pingus, Rib
Rohypnol Effects
- Amnesia
- Drowsiness
- Lower blood pressure
- Dizziness
- Confusion
- Stomach upsets
- Visual disturbances
- Inability to fight off a rapist
- Headaches
- Nightmares
- Muscle relaxation
- Tremors
- Loss of social restraints
Because Rohypnol is a benzodiazepine, withdrawal must be done carefully and under a doctor’s supervision. Withdrawal symptoms may include muscle pain, tension, loss of identity, delirium, shock and seizures.
LSD
While many people know that LSD was popular in the 1960s and 1970s, they may not know that LSD has recently made somewhat of a comeback. LSD is fairly popular at concerts and raves, but also at parties and on college campuses. The drug quickly causes distortions to perceptions of light, space, sound and time. A person may suffer a panic attack due to his ability to control his perceptions or environment which can lead to dangerous behavior. Uncontrollable hallucinations can lead to aggressive behavior or may lead the person to try some impossible action, like taking flight out of a second floor window.
LSD is sold in tablets or capsules but traditionally is distributed on small squares of blotter paper, often imprinted with a character or words. It may also be distributed as a liquid. The high of LSD is referred to as a trip. It may last as long as 12 hours.
LSD Effects
- Dilated pupils
- Increased body temperature
- Increased heart rate
- Dry mouth
- Shakiness
- Sweating
- Numbness
- Weakness
- Nausea
- Panic
- Terror
- Despair
- Swift emotional changes
- Hallucinations
- Delusions
Much later, a person may re-experience the effects of LSD, a phenomenon referred to as a flashback. These effects can come on with no warning at all and occur months or even a year or more later.
LSD is not physically addictive but it does produce a tolerance, which means that a person must take more of the drug to get the same effect that a smaller dose used to produce. Some people become psychologically addicted and cannot stop using this drug despite the harm it is doing.
LSD nicknames: Acid, Boomers, Yellow Sunshines, California sunshine, doses, dots, hippie, windowpane, tabs, blotters, battery acid, looney tunes.
Perhaps the worse effect of LSD is its ability to cause psychosis, either short-term or long-term. There have been cases where a person became psychotic or schizophrenic for a period of months, and others where the person did not recover.
Methamphetamine
Methamphetamine is a very strong stimulant. With some methods of administration, there is a fast “rush” of euphoria followed by a long period of less intense euphoria. When meth is ingested, there is no rush but the high may last for as long as ten hours.
Prescription Drugs And Their Uses
The user has more energy than normal and will not be able to sleep until the drug wears off. If he has plenty of the drug, he may continually re-dose until he has been up for days. If he runs out of the drug, he will crash and sleep around the clock. He will not have an appetite, meaning that he will probably lose a lot of weight. Heavy meth users become gaunt and look pale and unhealthy. He or she will probably appear unusually active but may also act nervous and anxious.
The user’s body temperature will go up and he may appear hot and sweaty without the environment being hot or his having been physically active. Pupils will be dilated and blood pressure will go up. He or she may become sexually excited.
Meth abuse results in the following adverse effects:
- Deterioration of appearance
- Irregular or speeded heartbeat
- Erratic, changeable moods
- Aggressive behavior
- Paranoia that can become severe
- Confusion
- Insomnia
- Damage to teeth
- Rough skin with sores
Meth is highly addictive. Some people have stated that just one or two uses was all it took for them to become addicted.
Slang terms for methamphetamine: Chalk, crank, crystal, ice, speed, white cross, tine, batu, LA glass, LA ice, quartz, junk, no doze, rocket fuel, scooby snax, cotton candy
The Other Synthetics
Chemical tests of substances sold as these drugs, especially Ecstasy, have shown that they are frequently adulterated with other substances. Here is some brief information on these other substances and their dangers.
Piperazines like BZP (1-benzylpiperazine) and TFMPP (1-(3-trifluoromethyl-phenyl)piperazine) among others: These drugs are often sold in blister packs. Users experience increased heart rate and blood pressure. Pupils dilate. They go hot and cold, have stomach pains and nausea, headaches and tremors. Some people experience severe seizures and others have panic attacks.
PMA/PMMA
(mostly found in the UK)
Chemical names:
- Para-methoxyamphetamine (PMA)
- Para-methoxymethamphetamine (PMMA)
- Chemically, these drugs are similar to Ecstasy or methamphetamine.
These are strong stimulants that cause increases in energy, body temperature, blood pressure and heart rate. They can also cause hallucinations, convulsions and respiratory distress. Some people have received PMA or PMMA when they thought they were getting Ecstasy and later died. Dozens of deaths have been associated with these two drugs.
Mephedrone
(mostly outside the US):
This drug is in a class called cathinones. It is chemically similar to amphetamine and produces a similar experience to amphetamine, methamphetamine, Ecstasy or cocaine. Users report euphoria and a sense of wellbeing, alertness and confidence. Adverse effects include racing heart, blurred vision, tension in face and jaw, blue fingers and other extremities, nausea, vomiting and a compulsion to continue to use it despite harm. Some people suffer hallucinations and insomnia. Use of mephedrone has been associated with a number of deaths, but the role of this drug in causing those deaths is uncertain.
MDPV
Known chemically as 3,4 methylenedioxypyrovalerone; This is also a cathinone and has similar effects as mephedrone but it is much more potent than other drugs in this class.
bk-MDMA (methylone)
This is one of the chemicals that may be used in “bath salts” or that may be found in a pill sold as Ecstasy. Use has been associated with the sudden death of otherwise healthy individuals. Users tend to overheat, have blurred vision and lose their ability to perceive time accurately. They may grind their teeth, be dizzy and confused and suffer hallucinations. Users sometimes report a feeling of empathy, similar to that of Ecstasy.
Be Drug Free. For Good.
J Adolesc Health. Author manuscript; available in PMC 2007 Jan 8.
Published in final edited form as:
Published online 2006 Oct 5. doi: 10.1016/j.jadohealth.2006.07.016
NIHMSID: NIHMS14399
The publisher's final edited version of this article is available at J Adolesc Health
See other articles in PMC that cite the published article.
Abstract
Purpose
The main objective of this study was to assess the prevalence of medical and nonmedical use of four categories of prescription drugs (opioid, stimulant, sleeping, and sedative/anxiety medication) in a racially diverse sample of secondary public school students in the Detroit metropolitan area. A secondary objective was to examine the association between the use of four categories of prescription medications and illicit drug use and probable drug abuse.
Methods
In 2005, a Web-based survey was self-administered by 1086 secondary school students in grades seven through 12.
Results
The sample consisted of 54% female, 52% White, 45% African American, and 3% from other racial categories. Forty-eight percent of the sample reported no lifetime use of four categories of prescription drugs (nonusers), 31.5% reported medically prescribed use only (medical users), 17.5% reported both medical and nonmedical use (medical/nonmedical users) and 3.3% reported nonmedical use only (nonmedical users). Multivariate analyses indicated that medical/nonmedical users and nonmedical users were significantly more likely than nonusers to report illicit drug use and probable drug abuse. Medical users generally reported similar or increased odds of illicit drug use and probable drug abuse than non-users.
Conclusions
These findings provide evidence that nonmedical use of prescription drugs represents a problem behavior among secondary school students.
Keywords: Prescription drugs, Epidemiology, Drug abuse, Adolescents, Survey research, School-based research
The medical and nonmedical use of prescription drugs such as benzodiazepines, opioid analgesics, and stimulants has increased among adolescents and young adults in the United States during the past decade [1–]. According to the Monitoring the Future Study (MTF), the nonmedical use of several prescription medications by 12th graders in the United States is at its highest level in the past 15 years [1,2]. Because prescription drugs are necessary for the treatment of many pediatric disorders including anxiety, sleep, and attention deficit hyperactivity disorder (ADHD), any examination of the nonmedical use and abuse of prescription drugs should occur within the larger context of proper medical use. With appropriate medical use considered, there are at least three studies that have examined nonmedical use among adolescents [–]; however, these earlier studies limited their focus to either stimulant or pain medications. To date, there are few (if any) investigations examining secondary students’ reports of medical and nonmedical use of all four of the most abused classes of prescription drugs (i.e., opioid, stimulant, sleeping, and sedative/anxiety medications).
In 2001, Poulin reported on a sample of secondary school students and found that nonmedical use of prescription stimulants was directly correlated to the number of prescription users in a particular school class who reported giving away their stimulant medication []. Although there were some limitations in the measures used by Poulin, the investigation represented one of the first attempts to examine medical and nonmedical use of prescription stimulants at the school class level []. In two subsequent studies, McCabe and colleagues reported that secondary school students who properly use prescription stimulant or pain medications were not at greater risk for substance use than nonusers [,]. For example, students who used their prescription stimulants for ADHD (e.g., Ritalin®, Adderall®, etc.) did not report higher rates of alcohol, marijuana, and other illicit drug use than nonstimulant-using peers; however, students who reported nonmedical use of prescription stimulants had significantly higher rates of alcohol, marijuana, and other illicit drug use when compared with students who did not use prescription stimulant medication []. These stimulant findings are similar to those reported by Boyd and colleagues for prescription opioid analgesics. Boyd and colleagues found that secondary students who reported medical use of prescription opioids (used as prescribed) were no more likely to use substances than their nonopioid-using counterparts; however, secondary school students who reported nonmedical use had significantly higher rates of alcohol, marijuana, and other illicit drug use than their nonopioid using counterparts []. Despite growing evidence suggesting significant associations between prescription medication use and other drugs, there is limited information regarding these associations among secondary students.
The current study builds on earlier studies and assesses medical and nonmedical use of four different classes of abusable prescription drugs (i.e., opioid, stimulant, sleeping, and sedative/anxiety medications) in a probability-based sample of secondary school students in a Detroit-area public school district. The specific objectives of this study were to examine the prevalence of the following: 1) medical use of four classes of prescription drugs, 2) nonmedical use of four classes of prescription drugs, and 3) illicit drug use and probable drug abuse based on use of four classes of prescription drugs.
Methods
The present study was conducted during a one-week period in May 2005, drawing on the entire population of 1594 middle school and high school students from a public school district in the Detroit metropolitan area (seventh through 12th grades). The study received approval from the University of Michigan Institutional Review Board and a Certificate of Confidentiality was obtained from the National Institutes of Health. All parents in the school district were sent letters explaining that their child’s participation was voluntary, describing the relevance of the study, and assuring that all responses would be kept confidential. Seventy-three percent of parents gave informed consent. The survey was conducted over the internet from school-based computer labs and students were excused from class to complete the survey. All participants were informed that a private research firm, unaffiliated with the school district, was contracted to set up the Web survey as well as store and maintain data to ensure students’ responses were kept completely confidential.
The Web-based survey method was used in part because computer-based approaches have been shown to have certain advantages relative to hardcopy surveys such as faster turnaround time and improved reporting of highly sensitive and illegal behaviors [,]. The Web survey was maintained on a hosted secure Internet site running under the secure sockets layer (SSL) protocol to insure respondent data were safely transmitted between the respondent’s browser and the server. Students were given sheets with a unique preassigned PIN number that allowed them to access the Web survey and these sheets were destroyed immediately after the survey administration; school officials and staff were unable to access any personally identifiable information connected with the data of any respondent. The survey took approximately 22 minutes to complete, and survey administration was supervised by staff from the University of Michigan, the public school district, and a private research firm. The project achieved a participation rate of 94% for students in the seventh through 12th grades whose parents gave informed consent, and the main reason for nonresponse was absenteeism on the days of survey administration. The final response rate for this Web-based survey was 68% based on guideline #2 of the American Association for Public Opinion Research (AAPOR); this guideline asserts that the response rate should be calculated by dividing the number of completed and partial cases by the number of all eligible respondents [17].
Measures
Medical use of prescription medication
Medical use of prescription medication was measured using the following question: “Based on a health professional’s (e.g., doctor, dentist, nurse) prescription, on how many occasions in your lifetime have you used the following types of drugs?” A separate question was asked for each of the following four classes of prescription drugs: (a) Sleeping medication (e.g., Ambien, Halcion, Restoril, temazepam, triazolam); (b) Sedative/anxiety medication (e.g., Ativan, Xanax, Valium, Klonopin, diazepam, lorazepam); (c) Stimulant medication for ADHD (e.g., Ritalin, Dexedrine, Adderall, Concerta, methlyphenidate); (d) Pain medication (i.e., opioids such as Vicodin, OxyContin, Tylenol 3 with codeine, Percocet, Darvocet, morphine, hydrocodone, oxycodone). The response scale for each question was (1) Never, (2) 1–2 occasions, (3) 3–5 occasions, (4) 6–9 occasions, (5) 10–19 occasions, (6) 20–39 occasions, and (7) 40 or more occasions.
Nonmedical use of prescription medication
Nonmedical use of prescription medication was assessed by asking the following question: “Sometimes people use prescription drugs that were meant for other people, even when their own health professional (e.g., doctor, dentist, nurse) has not prescribed it for them. On how many occasions in your lifetime have you used the following types of drugs, not prescribed to you?” There were separate questions for each of the following four classes of prescription drugs: (a) Sleeping medication (e.g., Ambien, Halcion, Restoril, temazepam, triazolam); (b) Sedative/anxiety medication (e.g., Ativan, Xanax, Valium, Klonopin, diazepam, lorazepam); (c) Stimulant medication for ADHD (e.g., Ritalin, Dexedrine, Adderall, Concerta, methlyphenidate); (d) Pain medication (i.e., opioids such as Vicodin, OxyContin, Tylenol 3 with codeine, Percocet, Darvocet, morphine, hydrocodone, oxycodone). The response scale for each question was the same as for medical use.
Prescription drug use status
Prescription drug use status was assessed by creating four distinct groups of lifetime prescription medication use: (1) individuals who never used one or more of the four classes of prescription medication (nonusers, n = 499); (2) individuals who only used one or more of the four classes of prescription medication as prescribed by their physicians (medical user only, n = 329); (3) individuals who used one or more of the four classes of prescription medication as prescribed by their physicians, as well as prescription medication that was not prescribed to them (both medical and nonmedical user, n = 183); (4) individuals who only used one or more of the four classes of prescription medication that was not prescribed to them (nonmedical user only, n = 35). Similar four-level indicator variables were developed for each specific drug class.
Drug Abuse Screening Test, Short Form (DAST-10)
The Drug Abuse Screening Test, Short Form (DAST-10) is a self-report instrument that can be used in clinical and non-clinical settings to screen for probable drug abuse or dependence on a wide variety of substances other than alcohol [17]. Respondents who used drugs other than alcohol in the past 12 months were asked whether they had experienced 10 drug-related items in the past 12 months (e.g., inability to stop using drugs, simultaneous polydrug use, illegal activities to obtain drugs, blackouts as a result of drug use, medical problems as a result of drug use, withdrawal symptoms, felt bad or guilty about drug use, family complaints about drug use, and family avoidance due to drug use). Based on the objectives of the present study, we removed the item regarding “non-medical reasons” for drug use resulting in nine DAST items. Based on previous research, if a respondent positively endorsed two or more DAST items, this was considered a “positive” screening test result, denoting risk for probable drug abuse or dependence [18–]. Cronbach’s alpha was .80 for the nine DAST items.
Data analysis
Data analyses included 1086 respondents, and all statistical analyses were performed using SPSS 13.0 (SPSS Inc., Chicago, IL). Chi-square tests were used to compare the prevalence of medical use and nonmedical use according to student characteristics. Chi-square tests and multiple logistic regression models were used to compare illicit drug use and DAST scores across the following four mutually exclusive groups of lifetime and past-year prescription medication users: (1) no use, (2) medical use only, (3) both medical and nonmedical use, and (4) nonmedical use only. Multiple logistic regression models used nonusers as the reference group and were adjusted for gender, race/ethnicity, and grade level. Interactions between demographic characteristics (e.g., gender, race/ethnicity, and grade level) were examined in the multiple logistic regression models. Adjusted odds ratios (AOR) and 95% confidence intervals (95% CI) were reported.
Sample
The final sample consisted of 1086 secondary school students, and the demographic characteristics resembled the characteristics of the overall student population. The grade level distribution did not significantly differ between the final sample (37% in seventh–eighth grade and 63% in ninth–12th grade) and the overall student population (35% in seventh–eighth grade and 65% in ninth–12th grade). The final sample contained a higher proportion of females (54%) than in the overall student population (51%) (χ2 = 10.5, df = 1, p < .01). The racial distribution of the final sample was 52% White, 45% African American, and 3% from other racial categories, whereas the racial distribution of the overall student population was 48% White, 49% African American, and 3% other racial categories (χ2 = 26.7, df = 2, p < .01).
Results
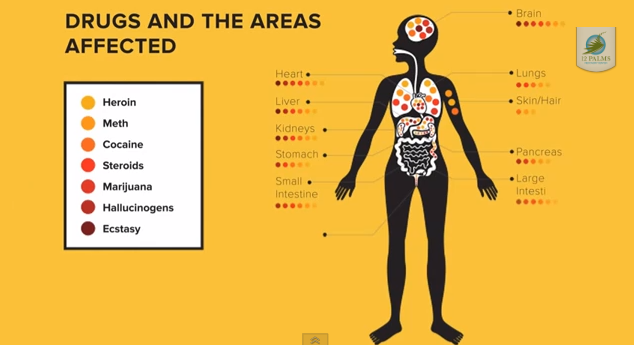
The lifetime prevalence of medical use was 49.0% for any of the four categories of prescription medications. The most common medically used prescription drug class among secondary school students was pain medication (44.9%), followed by sleeping (13.9%), sedative/anxiety (6.1%), and stimulant medications (6.0%). There were notable gender differences; within any of the four classes, females were significantly more likely than males to report lifetime medically prescribed use (56.4% vs. 40.2%, χ2 = 27.4, df = 1, p < .001), pain medication (53.1% vs. 35.0%, χ2 = 34.0, df = 1, p < .001), sleeping medication (16.2% vs. 11.2%, χ2 = 5.5, df = 1, p < .05), and sedative/anxiety medication (7.6% vs. 4.4%, χ2 = 4.5, df = 1, p < .05). There were also some significant racial differences; White students were significantly more likely than African American students to report medical use of sedative/anxiety medication (8.8% vs. 3.0%, χ2 = 14.2, df = 1, p < .001) and stimulant medication (8.0% vs. 3.5%, χ2 = 9.0, df = 1, p < .01). Older students in grades nine–12 were more likely than students in grades seven to eight to report medical use of sedative/ anxiety medication (7.3% vs. 4.1%, χ2 = 4.2, df = 1, p < .05) and pain medication (48.9% vs. 38.1%, χ2 = 11.4, df = 1, p < .01). The correlations among frequencies of lifetime medical and nonmedical use of prescription drugs ranged from .14 to .84, with most correlations between .30 and .50 (Table 1).
Table 1
Zero-order correlations between lifetime frequency of medical and nonmedical use of prescription drugs
| Variable | 1. | 2. | 3. | 4. | 5. | 6. | 7. | 8. | M | SD | Range |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. Frequency of lifetime stimulant medical use | -- | 1.21 | .99 | 1–7 | |||||||
| 2. Frequency of lifetime stimulant nonmedical use | .34** | -- | 1.07 | .55 | 1–7 | ||||||
| 3. Frequency of lifetime pain medical use | .18** | .14** | -- | 2.12 | 1.70 | 1–7 | |||||
| 4. Frequency of lifetime pain nonmedical use | .24** | .45** | .38** | -- | 1.37 | 1.03 | 1–7 | ||||
| 5. Frequency of lifetime sedative medical use | .46** | .51** | .23** | .33** | -- | 1.14 | .73 | 1–7 | |||
| 6. Frequency of lifetime sedative nonmedical use | .40** | .84** | .21** | .49** | .62** | -- | 1.09 | .60 | 1–7 | ||
| 7. Frequency of lifetime sleeping medical use | .34** | .31** | .38** | .36** | .43** | .48** | -- | 1.33 | 1.07 | 1–7 | |
| 8. Frequency of lifetime sleeping nonmedical use | .33** | .71** | .20** | .52** | .48** | .76** | .45** | -- | 1.15 | .73 | 1–7 |
Note: Sample sizes varied due to missing data (range = 1030–1046).
For any drug category studied, the lifetime prevalence of nonmedical use was 20.9%. The lifetime prevalence of nonmedical use was highest for pain medication (17.7%), followed by sleeping (5.9%), sedative/anxiety (3.5%), and stimulant medications (2.4%). Females were significantly more likely than males to report nonmedical use of pain medication (22.2% vs. 12.3%, χ2 = 17.6, df = 1, p < .001). White students were more likely than African American students to report nonmedical use of prescription sedative/ anxiety (4.5% vs. 2.2%, χ2 = 4.2, df = 1, p < .05) and stimulant medications (3.3% vs. 1.3%, χ2 = 4.2, df = 1, p < .05). Finally, students in grades nine–12 were more likely than students in grades seven to eight to report non-medical use of sedative/anxiety (4.5% vs. 1.8%, χ2 = 5.3, df = 1, p < .05) and pain medications (20.9% vs. 12.1%, χ2 = 12.9, df = 1, p < .001).
As illustrated in Table 2, approximately 48% (n = 499) of students never used an abusable prescription drug (lifetime nonuser), 31.5% (n = 329) used prescription medication as prescribed by their physicians (lifetime medical user only), 17.5% (n = 183) used both prescription medication as prescribed by their physicians as well as used an abusable prescription medication that was not prescribed to them (lifetime medical and nonmedical user), and 3.3% (n = 35) used an abusable prescription medication that was not prescribed to them (lifetime nonmedical user only).
Table 2
Frequency distributions of lifetime prescription drug use
| Lifetime prescription drug use status | Sample size (n) | Sample size (%) |
|---|---|---|
| Four classes of prescription drugsa | ||
| Nonuser | 499 | 47.7 |
| Medical user only | 329 | 31.5 |
| Medical and nonmedical user | 183 | 17.5 |
| Nonmedical user only | 35 | 3.3 |
| Pain medication | ||
| Nonuser | 535 | 51.9 |
| Medical user only | 313 | 30.4 |
| Medical and nonmedical user | 147 | 14.3 |
| Nonmedical use only | 35 | 3.4 |
| Sleeping medication | ||
| Nonuser | 872 | 83.9 |
| Medical user only | 106 | 10.2 |
| Medical and nonmedical user | 36 | 3.5 |
| Nonmedical user only | 25 | 2.4 |
| Sedative/anxiety medication | ||
| Nonuser | 964 | 92.7 |
| Medical user only | 39 | 3.8 |
| Medical and nonmedical user | 25 | 2.4 |
| Nonmedical user only | 12 | 1.2 |
| Stimulant medication | ||
| Nonuser | 962 | 92.9 |
| Medical user only | 50 | 4.8 |
| Medical and nonmedical user | 12 | 1.2 |
| Nonmedical user only | 12 | 1.2 |
aFour classes of prescription drugs include pain, sleeping, sedative/ anxiety and stimulant medications.
Bivariate analyses indicated significant gender differences in lifetime medical and nonmedical use of four classes of prescription drugs (Table 3). There were no significant racial differences in the lifetime use of prescription medication; predictably, grade level was significantly associated with lifetime use of prescription drugs.
Table 3
Demographic characteristics based on lifetime use of four classes of prescription drugs
| Differences based on chi-square | |||||
|---|---|---|---|---|---|
| Nonuser (n = 499) % | Medical use only (n = 329) % | Medical/nonmedical use (n = 183) % | Nonmedical use only (n = 35) % | χ2 (df) p-value | |
| Gender | |||||
| Female | 46.0 | 58.2 | 70.5 | 57.1 | 35.24 (3) p < .001 |
| Male | 54.0 | 41.8 | 29.5 | 42.9 | |
| Race/ethnicity | |||||
| White | 51.2 | 56.4 | 50.3 | 51.4 | NS |
| African American | 45.4 | 41.2 | 45.4 | 45.7 | |
| Other | 3.4 | 2.4 | 4.4 | 2.9 | |
| Grade level | |||||
| 7th–8th grade | 41.9 | 36.5 | 24.0 | 31.4 | 18.81 (3) p < .001 |
| 9th–12th grade | 58.1 | 63.5 | 76.0 | 68.6 | |
Bivariate analyses were used to examine the associations among lifetime prescription drug use, past-year illicit drug use, and DAST scores. Chi-square analysis revealed significant associations between lifetime prescription drug use status and each measure of past-year illicit drug use and probable drug abuse as measured by the DAST (p < .001). Multivariate logistic regression results reinforced the bivariate findings; the odds of reporting illicit drug use and probable drug abuse were considerably higher among individuals who reported lifetime nonmedical use only of prescription drugs after adjusting for gender, race/ethnicity and grade level (Table 4). The heightened risk for illicit drug use and probable drug abuse among lifetime nonmedical users of prescription drugs held steady across each of the four classes of prescription drugs. In addition, illicit drug use and probable drug abuse among individuals who reported both lifetime medical and nonmedical use of prescription drugs were similar to individuals who reported only lifetime non-medical use. Individuals who reported only lifetime medical use generally reported similar or increased odds of illicit drug use and probable drug abuse (DAST score) than individuals who reported no lifetime use of prescription drugs. Finally, we tested for interactions involving gender, racial/ ethnic, and grade level variables and generally found no evidence for interactions between these variables and prescription drug use status in accounting for probable drug abuse.
Table 4
Prevalence of drug use and misuse based on lifetime use of four classes of prescription drugs
| Past-year DAST (positive screening) two or more items | Past-year marijuana use | Past-year illicit drug use other than marijuanaa | ||||
|---|---|---|---|---|---|---|
| Prescription drug use status | % | AORb (95% CI) | % | AORb (95% CI) | % | AORb (95% CI) |
| Four prescription drug classesc | ||||||
| Nonuser | 5.0 | -- | 13.5 | -- | 2.6 | -- |
| Medical user only | 7.3 | 1.5 (.8–2.8) | 19.9 | 1.5 (1.0–2.2)* | 6.1 | 2.6 (1.3–5.4)** |
| Medical and nonmedical user | 20.9 | 5.2 (2.9–9.1)*** | 33.0 | 2.6 (1.7–4.0)*** | 12.0 | 6.5 (3.1–13.7)*** |
| Nonmedical user only | 22.9 | 6.7 (2.7–16.8)*** | 21.2 | 1.7 (.7–4.2) | 11.4 | 5.7 (1.7–19.1)** |
| Pain medication | ||||||
| Nonuser | 5.2 | -- | 13.7 | -- | 3.0 | -- |
| Medical user only | 8.0 | 1.6 (.9–2.8) | 21.7 | 1.6 (1.1–2.4)* | 5.8 | 2.3 (1.1–4.6)* |
| Medical and nonmedical user | 21.8 | 5.3 (3.0–9.4)*** | 33.3 | 2.6 (1.6–4.1)*** | 12.2 | 5.9 (2.8–12.4)*** |
| Nonmedical use only | 22.9 | 6.1 (2.5–15.2)*** | 18.2 | 1.3 (.5–3.4) | 14.3 | 6.4 (2.1–19.3)** |
| Sleeping medication | ||||||
| Nonuser | 6.7 | -- | 16.5 | -- | 3.7 | -- |
| Medical user only | 14.2 | 2.4 (1.3–4.5)** | 30.0 | 2.5 (1.6–4.2)*** | 9.4 | 2.7 (1.3–5.8)* |
| Medical and nonmedical user | 44.4 | 11.0 (5.3–23.0)*** | 45.7 | 4.4 (2.1–9.3)*** | 30.6 | 12.4 (5.4–28.2)*** |
| Nonmedical user only | 25.0 | 5.8 (2.1–16.0)** | 33.3 | 3.6 (1.4–9.1)** | 24.0 | 9.0 (3.2–25.0)*** |
| Sedative/anxiety medication | ||||||
| Nonuser | 7.4 | -- | 17.2 | -- | 4.4 | -- |
| Medical user only | 15.4 | 2.2 (.9–5.7) | 28.9 | 1.6 (.8–3.5) | 7.7 | 2.1 (.6–7.4) |
| Medical and nonmedical user | 54.2 | 14.6 (6.0–35.4)*** | 68.0 | 8.9 (3.6–22.2)*** | 44.0 | 23.3 (9.2–59.1)*** |
| Nonmedical user only | 41.7 | 8.7 (2.6–29.3)*** | 41.7 | 3.1 (1.0–10.3) | 25.0 | 7.6 (1.9–31.1)** |
| Stimulant medication | ||||||
| Nonuser | 6.5 | -- | 17.2 | -- | 4.0 | -- |
| Medical user only | 30.0 | 6.0 (3.0–11.8)*** | 27.1 | 1.7 (.9–3.5) | 14.0 | 3.5 (1.4–8.4)** |
| Medical and nonmedical user | 72.7 | 31.0 (7.7–125.1)*** | 91.7 | 52.0 (6.1–439.8)*** | 58.3 | 36.7 (10.4–130.2)*** |
| Nonmedical user only | 75.0 | 44.5 (11.3–174.9)*** | 66.7 | 11.9 (3.4–42.3)*** | 50.0 | 22.4 (6.7–74.5)*** |
aPast-year illicit drug index consists of summing annual use of cocaine, LSD, other psychedelics, inhalants, ecstasy, crystal methamphetamine, heroin, and GHB.
bOdds ratios (AOR) are adjusted for gender, race/ethnicity and grade level (odds ratios for these variables were not shown).
cFour classes of prescription drugs included pain, stimulant, sleeping, and sedative/anxiety medications.
**p < .01;
The past-year use of four classes of prescription drugs was as follows: 59.7% (n = 623) of students never used an abusable prescription drug (past-year nonuser), 26.5% (n = 276) used prescription medication as prescribed (past-year medical user only), 10.6% (n = 111) used both prescription medication as prescribed as well as an abusable prescription medication that was not prescribed (past-year medical and nonmedical user), and 3.2% (n = 28) used an abusable prescription medication that was not prescribed (past-year nonmedical user only). The association between past-year prescription drug use status and probable drug abuse was examined using chi-square analysis that revealed significant associations (p < .001). The prevalence of experiencing two or more DAST items was 5.5% among past-year nonusers, 6.9% for past-year medical users only, 29.1% for past-year medical and nonmedical users and 27.3% for past-year nonmedical users only.
The logistic regression results supported the bivariate findings because the odds of experiencing two or more DAST items did not differ significantly between past-year medical users and past-year nonusers after adjusting for gender, race/ethnicity, and grade level. In contrast, past-year medical and nonmedical users were over seven times more likely than past-year nonusers to experience two or more DAST items (AOR = 7.7, 95% CI = 4.3–13.7, p < .001). Similarly, past-year nonmedical users were over seven times more likely than past-year nonusers to experience two or more DAST items (AOR = 7.6, 95% CI = 3.2–18.4, p < .001).
Finally, we examined whether higher frequencies of non-medical use of each prescription drug class (lifetime and past-year) were positively associated with illicit drug use and probable drug abuse (lifetime and past-year). Bivariate correlations revealed significant positive associations between frequencies of nonmedical use for each class of prescription drugs and illicit drug use and probable drug abuse (p < .001).
Discussion
In the present study, the lifetime prevalence rate of non-medical use within the four prescription drug classes was 20.9%; this was higher than the lifetime prevalence of nonmedical use for the same four prescription drug classes (13.5%) among persons 12 to 17 years of age nationally in 2004 [3]. Notably, the prevalence of nonmedical use of prescription opioids was higher than state and national averages, whereas the prevalence of nonmedical use of prescription stimulants was lower [1,3,21,]. For example, in this study the lifetime prevalence of nonmedical use of prescription opioids was 17.7% and this is contrasted to national and state data that indicate 11.4% of persons 12 to 17 years and 14.3% of Michigan residents (12 years or older) reported lifetime nonmedical use of prescription opioids [1,21].
The lifetime prevalence rates of medical use of prescription drugs reported here were similar to the prevalence rates and increasing prescribing patterns for U.S. youth [,–]. For example, the lifetime prevalence of medical use of prescription stimulants for ADHD was 6.0% in the present study; this is similar to data that suggest 5.0% of youth aged 5 to 17 years in the state of Michigan [] and 4.3% of U.S. youth between 4 and 17 years of age are prescribed stimulant medication []. The gender differences in medical use of prescription drugs resembled national patterns [,,]; adolescent girls were more likely to report medical use of prescription opioids, sedative/anxiety medication, and sleeping medication. We also found boys were more likely to report medical use of prescription stimulants for ADHD, but the difference was not statistically significant. Although these gender differences have been found in prescribing patterns in previous research with secondary school students, these prior studies did not consider the association with nonmedical use.
Seven of every 10 secondary students who reported medical and nonmedical use of prescription drugs were female. The increased rates of nonmedical use among female medical users could be the result of greater medical exposure to medications or, alternatively, it could be due to possible under-treatment of conditions that result in girls obtaining prescription medications from friends, family members, or others to self-treat. After all, the leading sources of prescription drugs among adolescent nonmedical users are peers and family members [,,], and this suggests that nonmedical use among adolescents should be considered within the larger context of medical availability.
The racial differences in medical and nonmedical use of prescription drugs found here are notable relative to previous research. The higher rates of medical and nonmedical use of stimulant and sedative/anxiety medications among White youth were similar to the racial differences in both prescribing patterns [–] and nonmedical use of stimulant medications [1,,]. Although we found no difference between White and African American students, national findings indicate lifetime nonmedical use of prescription opioid medications was higher among White 12th grade students (15.9%) than among African American (3.5%) 12th grade students [1]. Furthermore, we did not find any racial differences in lifetime medical and nonmedical use when considering all four classes of prescription drugs. We also did not observe differences by grade level in lifetime medical or nonmedical use of stimulant and sleeping medications; this could be the result of increased prescription rates of these classes of drugs among younger students. Our findings serve as a reminder that secondary school districts should be encouraged to collect data to learn more about drug use behaviors because national results may not hold true in their respective schools.
Our data indicate that nonmedical use of prescription drugs represents a problem behavior among secondary school students. Approximately one in every five secondary school adolescents reported nonmedical use of prescription drugs and these youth were at greater risk for probable drug abuse or dependence than their peers. This study also found that a higher frequency of nonmedical use of prescription drugs is positively associated with probable drug abuse or dependence. The high rates of drug-use-related problems among nonmedical users of prescription medication provide support for targeting prescription drug abuse in prevention and intervention efforts among adolescents.
The present study contained several strengths and limitations that should be considered. A major strength pertains to the diversity of the sample, with 45% of the students identifying as African American. However, based on the racial diversity of the school district, some caution should be used when comparing the findings of the present study to other school districts that are less diverse. An additional strength of the present study was the inclusion of several classes of prescription medications and of screening items to detect probable drug abuse or dependence. Many previous studies focus exclusively on one class of prescription drugs and fail to take into account medical and nonmedical use of other classes of abusable prescription drugs.
Approximately three in every 10 students in the school district failed to complete the survey and this may lead to biased findings; however, concern regarding nonresponse bias was somewhat lessened because the demographic characteristics of the final sample resembled the student population. Some of our analyses were limited by the small number of students who reported medical and nonmedical use of some prescription drugs. Finally, although the DAST has been used in clinical and nonclinical settings, the instrument has not been used widely in adolescent populations. Further validation of the DAST using Web-based survey research and standard clinical interviews is needed to confirm optimal cut-points for sensitivity and specificity among adolescents.
Despite these limitations, the results of the present study indicate that medical users who used their prescription medications as intended were not at the same risk for probable drug abuse as individuals who reported both medical and nonmedical use, or those who reported nonmedical use only. This finding reinforces the importance of proper medical use of prescription drugs and reinforces the need for educational efforts directed at patients and their families. Data from the present study also support the importance of compliance with medication management and suggest that proper medical monitoring may be helpful in reducing non-medical use of prescription drugs by adolescents.
Acknowledgments
This study and development of this manuscript was supported by research grants DA018239 and DA018271 from the National Institute on Drug Abuse and AA014601 from the National Institute of Alcohol Abuse and Alcoholism, National Institutes of Health. The authors would like to thank the three anonymous reviewers for their helpful comments on an earlier version of this manuscript.
References
1. Johnston LD, O’Malley PM, Bachman JG, et al. Monitoring the Future National Survey Results on Drug Use, 1975–2004. Volume I: Secondary School Students. Bethesda, MD: National Institute on Drug Abuse; 2005. [Google Scholar]
2. Johnston LD, O’Malley PM, Bachman JG, et al. Monitoring the Future National Results on Adolescent Drug Use: Overview of Key Findings, 2005. Bethesda, MD: National Institute on Drug Abuse; 2006. [Google Scholar]
3. Substance Abuse Mental Health and Services and Administration. Results from the 2004 National Survey on Drug Use and Health: Detailed Tables. Rockville, MD: Office of Applied Studies, 2003 and 2004; [cited 2005 Dec 23]. Available from: http://oas.samhsa.gov/nsduh/2k4nsduh/2k4tabs/2k4tabs.pdf. [Google Scholar]
4. Joranson DE, Ryan KM, Gilson AM, et al. Trends in medical use and abuse of opioid analgesics. JAMA. 2000;283:1710–4. [PubMed] [Google Scholar]
5. Mohler-Kuo M, Lee JE, Wechsler H. Trends in marijuana and other illicit drug use among college students: results from 4 Harvard School of Public Health College Alcohol Study surveys: 1993–2001. J Am Coll Health. 2003;52:17–24. [PubMed] [Google Scholar]
6. Olfson M, Marcus SC, Druss B, et al. National trends in the use of outpatient psychotherapy. Am J Psychiatry. 2002;159:1914–20. [PubMed] [Google Scholar]
7. Olfson M, Gameroff MJ, Marcus SC, et al. National trends in the treatment of attention deficit hyperactivity disorder. Am J Psychiatry. 2003;160:1071–7. [PubMed] [Google Scholar]
8. Robison LM, Sclar DA, Skaer TL, et al. National trends in the prevalence of attention-deficit/hyperactivity disorder and the prescribing of methylphenidate among school-age children: 1990–1995. Clin Pediatr. 1999;38:209–17. [PubMed] [Google Scholar]
9. Robison LM, Skaer TL, Sclar DA, et al. Is attention deficit hyperactivity disorder increasing among girls in the US? Trends in diagnosis and the prescribing of stimulants. CNS Drugs. 2002;16:129 –37. [PubMed] [Google Scholar]
10. Zacny J, Bigelow G, Compton P, et al. College on Problems of Drug Dependence taskforce on prescription opioid non-medical use and abuse: position statement. Drug Alcohol Depend. 2003;69:215–32. [PubMed] [Google Scholar]
11. Zito JM, Safer DJ, DosReis S, et al. Psychotropic practice patterns for youth: a 10-year perspective. Arch Pediatr Adolesc Med. 2003;157:17–25. [PubMed] [Google Scholar]
12. Boyd CJ, McCabe SE, Teter CJ. Medical and nonmedical use of prescription pain medication by youth in a Detroit-area public school district. Drug Alcohol Depend. 2006;81:37–45.[PMC free article] [PubMed] [Google Scholar]
13. McCabe SE, Teter CJ, Boyd CJ. The use, misuse and diversion of prescription stimulants among middle and high school students. Subst Use Misuse. 2004;39:1095–116. [PubMed] [Google Scholar]
14. Poulin C. Medical and nonmedical stimulant use among adolescents: from sanctioned to unsanctioned use. CMAJ. 2001;165:1039–44.[PMC free article] [PubMed] [Google Scholar]
15. McCabe SE, Boyd CJ, Couper M, et al. Mode effects for collecting alcohol and other drug use data: Web and U.S. mail J Stud Alcohol. 2002;63:755–61. [PubMed] [Google Scholar]
16. Turner CF, Ku L, Rogers SM, et al. Adolescent sexual behavior, drug use, and violence: increased reporting with computer survey technology. Science. 1998;280:867–73. [PubMed] [Google Scholar]
17. American Association for Public Opinion Research. Standard definitions: final dispositions of case codes and outcome rates for surveys. 2004. [cited 2006 Mar 20]. Available from: http://www.aapor.org/pdfs/standarddefs_ver3.pdf.
18. Cocco KM, Carey KB. Psychometric properties of the Drug Abuse Screening Test in psychiatric outpatients. Psychol Assess. 1998;10:408–14.[Google Scholar]
19. Skinner H. The drug abuse screening test. Addict Behav. 1982;7:363–71. [PubMed] [Google Scholar]
20. French MT, Roebuck MC, McGeary KA, et al. Using the drug abuse screening test (DAST-10) to analyze health services utilization and cost for substance users in a community-based setting. Subst Use Misuse. 2001;36:927–46. [PubMed] [Google Scholar]
21. Substance Abuse Mental Health and Services and Administration. National Survey on Drug Use and Health, 2002, 2003, and 2004. Rockville, MD: Office of Applied Studies; [cited 2005 Nov 22]. Available from: http://drugabusestatistics.samhsa.gov/statesLatest.htm. [Google Scholar]
22. McCabe SE, Teter CJ, Boyd CJ, et al. Prevalence and correlates of illicit methylphenidate use among 8th, 10th, and 12th grade students in the United States, 2001. J Adolesc Health. 2004;35:501–4. [PubMed] [Google Scholar]
23. Cox ER, Motheral BR, Henderson RR, et al. Geographic variation in the prevalence of stimulant medication use among children 5 to 14 years old: results from a commercially insured US sample. Pediatrics. 2003;111:237–43. [PubMed] [Google Scholar]
24. Safer DJ, Malever M. Stimulant treatment in Maryland public schools. Pediatrics. 2000;106:533–9. [PubMed] [Google Scholar]
25. Centers for Disease Control and Prevention (CDC) Mental health in the United States: prevalence of diagnosis and medication treatment for attention-deficit/hyperactivity disorder—United States, 2003. MMWR. 2005;54:842–7. [PubMed] [Google Scholar]
26. Simoni-Wastila L. The use of abusable prescription drugs: the role of gender. J Womens Health Gend Based Med. 2000;9:289–97. [PubMed] [Google Scholar]
27. McCabe SE, Boyd CJ. Sources of prescription drugs for illicit use. Addict Behav. 2005;30:1342–50.[PMC free article] [PubMed] [Google Scholar]
28. McCabe SE, Teter CJ, Boyd CJ. Illicit use of prescription pain medication among college students. Drug Alcohol Depend. 2005;77:37–47. [PubMed] [Google Scholar]